Jennifer A. Belsky, MS, DO; and Amber M. Brown, MS, DO
In this study, the authors investigated the safety and feasibility of osteopathic manipulative treatment in a pediatric oncology inpatient setting.
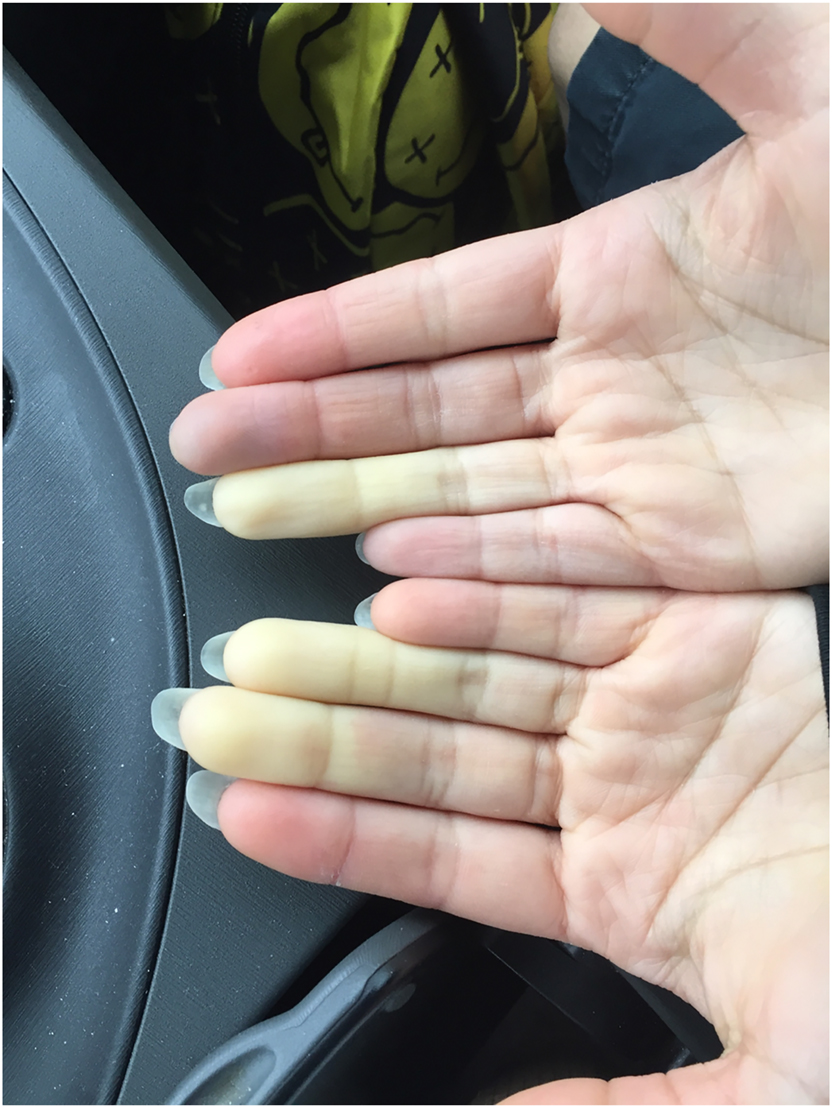
Clinical Image
Allison Kowalski, BS; and Robert Dazé, DO, FAAD
Medical Education
Anna N. Kirby, PhD, RD, LD, CCMS; Joy DeBellis, DNP, RN; Katie Wolter, MD; Gary Mount, PharmD; Chih-hsuan Wang, PhD; Jonathan Bishop, BS; Jessica Barkhouse, BS; Kathryn Wirth, BEng; Nancy Nguyen, MS; Christopher Cacciatore, BS; and Kristyn Kraus, BS
The objective of this study is to determine whether implementing a culinary medicine elective among medical and nurse practitioner students will increase their nutrition literacy and proficiency in counseling patients.